(News Release) The Lancet publishes important new study showing success of model of care in our NICU

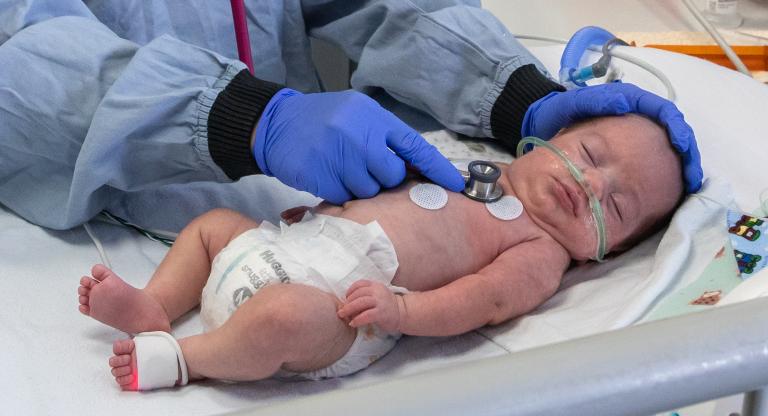
A new study by Mount Sinai neonatologist Dr. Karel O’Brien, and principal investigator, Dr. Shoo Lee, Chief of Pediatrics, published in the prestigious journal The Lancet Child & Adolescent Health shows that the Family Integrated Care (FICare) model of treating the tiniest and most fragile babies in Mount Sinai’s Newton Glassman Charitable Foundation Neonatal Intensive Care Unit helps improve the well-being of both children and parents. Family Integrated Care actively involves parents in the care of their newborns, including giving oral medicine, feeding, taking their temperatures and taking part in ward rounds.
The study, which involved 26 NICU units in Canada, Australia and New Zealand which had adopted the model of care developed at Mount Sinai Hospital by Dr. Lee, showed improved weight gain among preterm infants, better breastfeeding and reduced parental stress and anxiety compared to standard care.
“How care is provided to the family, not just the infant, has a positive effect on the wellbeing of both infant and family,” says Dr Karel O’Brien, who leads the Family Integrated Care Program at Mount Sinai. “Weight gain, breastfeeding and reduced parental stress and anxiety are all associated with positive neurodevelopmental outcomes, suggesting that integrating parents into the care of infants at this early stage could potentially have longer-term benefits.”
Mount Sinai supports parents in spending six hours a day, at least five days a week with their babies by providing them with with a rest space and sleeping room, comfortable reclining chairs at the bedside and nurses trained in family support.
At 21 days, infants in the FICare group had put on more weight and had higher average daily weight gain (26.7g vs 24.8g), compared to the standard care group. Additionally, parents in the FICare group had lower levels of stress and anxiety, compared to the standard care group. Once discharged, mothers were more likely to breastfeed frequently (more than 6 feeds a day), compared to the standard care group (70% vs 63% ). There were no differences in rates of mortality, duration of oxygen therapy or hospital stay.
“Parents are too often perceived as visitors to the intensive care unit. Our findings challenge this approach and show the benefits to both infants and their families of incorporating parents as key members of the infant’s health care team, and helping parents to assume the role of primary caregiver as soon as possible,” says Dr O’Brien.

“The results of this trial are encouraging indeed. Not only is this an example of innovative care developed here in our hospital, it is an exceptional example of how a good idea can be shared across the country and around the world,” says Dr. Lee, Chief of Pediatrics at Sinai Health System. “This was truly a collaborative effort with participating NICUs, parents, and the whole care team.”
When Amy, a new mother of twins found herself in the NICU with babies born at 23 weeks, 5 days, she felt scared and overwhelmed by how fragile the babies were. Today, still in the NICU for almost three months, she has found comfort in being part of the Ficare model of care. “It really allowed me to feel like a mother. Being with my babies all day, I know instinctively if something is wrong or what they need, and can report that to the doctors and nurses. They are getting stronger and stronger every day, and this model of care has made me believe that when I bring them home, I’ll be able to confidently care for them.”